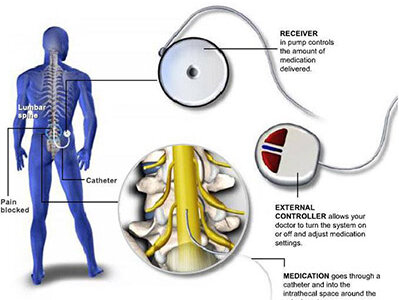
Administration of drug into the subarachnoid space, directly acts on the target receptors present on the dorsal horn cells which are responsible for pain transmission.
The intrathecal administration, allows the drug to bypass the enteric circulation/ absorption or the blood brain barrier hence the drug dose required for it , is a fraction of systemic dose with improved efficacy and hence minimized side-effects.
For example, the dose of baclofen from oral to intrathecal route decreases from approximately 300mg to 1mg. This continuous drug delivery system ensures a steady amount of drug level in blood, improving quality of analgesia. This is a modality which provides more effective pain relief.
There are a number of drugs which can be used with the system but the three drugs which are at present FDA approved are: Morphine, Baclofen and Ziconotide.
The Intrathecal drug pump system is a very sophisticated and programmable system.
It involves two stages. First is a trial phase, which is important to determine whether this particular system will suit the individual patient or not. It is just like test driving a car before buying it. Trial is performed to assess the patient’s response to the spasticity and improvement in side effects.
We perform trial by using intradural catheter (not bolus), which is implanted in strict aseptic conditions at the desired target site of the patient. The patient is then assessed for the improvement in spasticity of the target areas after 2, 4 and 6 hours.
We usually observe the patient in ICU during this time for better patient safety. If the trial is successful, we proceed for the implantation. After implantation the system is programmed accordingly to offer long lasting benefit in terms of satisfactory control of pain and spasticity.
The implantation of baclofen pump is performed in OT using fluoroscopic guidance and all surgical asepsis precautions.
The two pieces of silicone catheter is introduced through a special introducer needle and guided into the subarachnoid space up to the desired level depending upon the pain geography and properties of the drug used. It is then secured to the thoracolumbar fascia with special anchor, tunnelled in the subcutaneous plane and connected to the Synchro-med pump by suture less connector on the proximal piece of the catheter.
The pump is then emptied of its manufacturing fluid and filled with the desired drug to be administered before implanting in the subcutaneous pocket. Both the incisions are then surgically sutured after adequate haemostasis.
The Intrathecal pump is available in two main types, fixed rate [Isomed] and programmable [Synchromed] pump. The Synchromed pump has two varieties, an older Synchromed El and a newer Synchromed II system.
The Synchromed II has been an improved version and has been more popular due to its features such as lighter and flatter implant, increased drug stability upto 6 months and improved low reservoir flow accuracy.
It comes in two different sizes, 20ml and 40ml reservoir capacity. Improved software of Synchromed II stores all the patients demographics and notes up to 1000 characters. It can also stores catheter information and system log with last 30 events and the patient activation log of last 80 events.
This information is more useful when technical support is required for help. The information is presented in a scrollable window to accommodate more information with the multiple drugs. New software also allows drug data up to 5 drugs with the first drug as a primary drug.
A personal therapy manager (PTM) is a compact device which enable the patient to take extra boluses if required for the incidental or breakthrough pain. This gives a better degree of patient satisfaction.