More than 150,000 patients have undergone DBS. The present day techniques make it a very safe procedure.
Welcome to Jaslok Hospital, a place where compassionate care meets cutting-edge technology. If you or your loved ones are struggling with neurological disorders like movement disorders, e.g. Parkinson’s disease, tremors, etc or psychiatric disorders like severe depression or obsessive compulsive disorders, that have not responded well to conventional treatments, then Deep Brain Stimulation (DBS) may be the ray of hope you’ve been searching for. Our team of expert doctors and state-of-the-art facilities have earned us a stellar reputation as the best Deep Brain Stimulation center in Mumbai/ India.
Jaslok Hospital has been a leader in the field of tertiary care, and multi-specialty healthcare for over the decades. With an eye toward excellence and innovation, we provide world-class medical services that prioritize the patient. At Jaslok Hospital we have a dedicated Department of Neurological Surgery with the team of doctors who provide the best Deep Brain Stimulation in India and specialize in other neurosurgery treatments. Our Deep Brain Stimulation doctor have performed many DBS procedures for a variety of diseases, with excellent outcomes and high levels of satisfaction.
Deep Brain Stimulation (DBS) involves the implantation of a neurostimulator device that sends electrical impulses to definite targets inside the brain, i.e. the different brain nuclei & stimulates neurons located in it through implanted electrodes.

The DBS system consists of DBS leads containing four to eight electrodes or contact points that are implanted into the precise targets deep inside the brain. The lead emerges through a burr hole on the skull, connecting to an extension wire that eventually links to an electrical pulse generator (also called a pacemaker), preferably implanted under the skin over the left side chest wall.
DBS works by delivering the electrical impulses to the target areas & thus exerts its therapeutic effect.
Deep Brain Stimulation is much superior to the ablative surgeries for Parkinson’s disease and various other movement disorders. Subthalamic nucleus (STN), Globus pallidus internus (GPI) & Ventro-intermedius(VIM) nucleus of thalamus are structures within the brain that are targeted for Parkinson’s disease, dystonia & tremor respectively, although each of these target sites can be used interchangeably for different movement disorders.
Deep Brain Stimulation (DBS) has become a lifeline in the treatment of advanced Parkinson’s disease (PD) in the last decade. It’s associated with minimal morbidity & there are noticeable improvements in motor functions and quality of life in PD patients.
Around the world, DBS surgery has been performed on more than 2,50,000 patients of PD with remarkable improvements.
Deep Brain Stimulation procedures are more complex than conventional stereotactic techniques & require additional expertise that is required for routine functional neurosurgical procedures for different movement disorders.
A thorough understanding of the principles of DBS, knowledge regarding the disease being treated, and merging the medical therapy with stimulation is required to achieve smooth control of the disease.
Jaslok Hospital & Research Centre has been highly successful in developing a multi-disciplinary team approach for the smooth conductance of this surgery.
To learn more, you can visit our YouTube channel.

The multi-disciplinary team comprises of a skilled leading neurosurgeon, neurologist, clinical research fellow, Parkinson’s disease nurse, neuro-psychiatrist, and physiotherapist.
Expertise of speech therapists, occupational therapists and other specialists is also obtained whenever required.
The success of DBS largely dependent upon the selection of the appropriate patients as well as the accurate implantation of the stimulation electrodes, that necessitates careful imaging-based pre-targeting, extensive electro-physiological exploration of the targets during surgery & carefully executed individualised post-operative programming.
Deep Brain Stimulation is a revolutionary medical procedure that has transformed the lives of countless individuals battling neurological disorders, such as Parkinson’s disease, essential tremor, and dystonia. The DBS can also help in treateing the symptoms of psychiatric disorders like OCD and depression. It involves the use of a neurostimulator, commonly referred to as a brain pacemaker, which delivers electrical impulses to specific areas of the brain, modulating abnormal neuronal activity and alleviating symptoms.
When it comes to Deep Brain Stimulation treatment in Mumbai, Jaslok Hospital excels in providing state-of-the-art facilities and unmatched expertise. Our team of top Deep Brain Stimulation doctors in Mumbai and renowned neurologists, neurosurgeons, other healthcare professionals work collaboratively to ensure each patient receives personalized care and tailored treatment plans.
The Deep Brain Stimulation clinic at our hospital has been treating various conditions, including:
Deep Brain Stimulation (DBS) is a treatment option for people who have neurological problems that interfere with their movement, emotions, or other activities. However, DBS is not appropriate for everyone with these diseases. There are certain parameters for determining who might benefit from this surgery.
Here are some general DBS criteria that our Deep Brain Stimulation doctors in Mumbai check to determine whether the person is a good candidate for a Deep Brain Stimulator or not.
Some of the specific criteria for DBS vary depending on the condition being treated. For example:
Our experienced medical team thoroughly evaluates each patient’s medical history, symptoms, and lifestyle factors to decide if he or she is a good candidate for deep brain stimulator or not.
One of the aspects that set Jaslok Hospital apart is our unwavering commitment to our patients’ well-being. We not only ensure a seamless surgical experience but also provide comprehensive post-operative care and rehabilitation programs. Our experts guide patients through the recovery process, making sure they adapt smoothly to life after Deep Brain Stimulation surgery.
Some of the aspects of life after Deep Brain Stimulation surgery are:
After undergoing DBS surgery, patients typically spend a few days in the hospital for observation and recovery. They may experience some discomforts like pain, swelling, bruising, or incision site infection. Medication and proper wound care can effectively manage these. Patients may also experience temporary side effects such as headaches, nausea, dizziness, tingling, speech difficulties, or mood changes due to stimulation. Adjusting the settings of the neurostimulator device can often address these issues.
Fine-tuning the settings of the neurostimulator is a critical aspect of DBS treatment. A neurologist or a trained nurse typically carries out this optimization process using a handheld device that communicates with the neurostimulator. It might take multiple sessions to achieve the best results. Furthermore, patients or their caregivers can perform basic programming at home using a remote control device. Our Deep Brain Stimulation DBS doctors in Mumbai can also make adjustments remotely through a wireless system connected to the internet.
While DBS can significantly reduce the need for medication in some cases, it doesn’t entirely replace it. Especially in the early stages after surgery, patients may still require medication to manage their condition. The dosage and frequency of medication may be adjusted by the Deep Brain Stimulation DBS doctors based on the response to stimulation. It’s crucial for patients not to alter or discontinue their medication without consulting their doctor.
DBS can notably enhance a patient’s quality of life by reducing symptoms and improving day-to-day functioning. This includes positive effects on mood, cognition, sleep, and social interactions. However, it’s important to remember that DBS isn’t a cure, and patients may still face certain challenges. They might need to make lifestyle adjustments like maintaining a healthy diet, regular exercise, stress management, avoiding alcohol and tobacco, and considering psychological counseling if necessary.
Regular follow-ups and monitoring by the medical team at our Deep Brain Stimulation center in Mumbai are essential to ensure the safety and effectiveness of the stimulation. Patients will require periodic check-ups, tests, and programming adjustments. Any alterations in symptoms, side effects, or device function should be promptly reported to the Deep Brain Stimulation DBS doctors in Mumbai. Additionally, depending on usage and model, the battery of the neurostimulator device may need replacement every few years, which may necessitate another minor procedure or surgery.
The success of Deep Brain Stimulation largely depends on the proficiency of the medical team and the patient’s suitability for the procedure. The Deep Brain Stimulation clinic in Mumbai at Jaslok Hospital boasts an impressive success rate in DBS surgeries, which has garnered us a reputation for being a center of excellence in neurological care.
The Deep Brain Stimulation success rate depends on several factors, such as:
Different conditions have different responses to DBS. For example, DBS can reduce tremor by 80% to 90% in patients with essential tremor, improve motor function by 50% to 60% in patients with Parkinson’s disease, decrease seizure frequency by 50% to 70% in patients with epilepsy, reduce compulsions by 40% to 60% in patients with OCD, and improve dystonia symptoms by 50% to 70% in patients with dystonia.
DBS helps different parts of the brain in different ways. For example, it can ease problems with movement by gently nudging spots like the subthalamic nucleus (STN) or the globus pallidus internus (GPi). When we stimulate the anterior thalamic nucleus (ATN) or the hippocampus, it can reduce seizures. To lift up mood disorders, we focus on the ventral capsule/ventral striatum (VC/VS) or the subgenual cingulate gyrus (SCG). And to ease OCD symptoms, we target the internal capsule (IC) or the ventral globus pallidus (VGP).
The Deep Brain Stimulation success rate also depends on a few settings. Think of it like adjusting a radio. We set how often it sends signals (frequency), how strong those signals are (intensity), how long each signal lasts (pulse width), and how often it happens (duration). Getting these just right in the neurostimulator device is really important. It’s like tuning an instrument to make beautiful music.
Each person is like a puzzle, with different pieces that matter. Things like how old they are, if they’re a man or a woman, their medical history, the medicines they take, how they live, and what they hope for, all have a say. They can change how a person feels about the treatment, how comfortable they are with the procedure, and how well they stick to the follow-up care. Also, these factors can influence how happy a person feels and how good their life is after DBS.
Explore the pros and cons of Deep Brain Stimulation in our insightful blog post: Deep Brain Stimulation: Pros and Cons
There are multiple factors that influence the cost of DBS surgery, such as:
At Jaslok Hospital, the deep brain stimulation cost in Mumbai starts from ₹13.5 lakhs and can range up to ₹30 lakhs, depending on the patient’s condition and the chosen implant. to know more about prize in detail visIT our DBS Surgery Cost Page
Although Deep Brain Stimulation is considered a safe procedure, it is essential to understand potential long-term side effects.
It takes a few weeks to activate the device and determine the best settings for each person. Changing the device’s settings accordingly can fix adverse effects that may occasionally occur in certain settings.
The team our Deep Brain Stimulation clinic in Mumbai educates patients about the risks involved and implements stringent safety measures throughout the treatment journey to minimize any adverse outcomes.
Understanding the financial elements of DBS treatment is critical for anyone thinking about undergoing this life-changing technique. The costs are influenced by the specific condition being treated, the complexity of the procedure, and post-operative care requirements. During the initial consultation, our Deep Brain Stimulation clinic team at Jaslok Hospital is committed to giving honest, tailored cost estimates, ensuring that individuals have a clear idea of the financial commitment needed.
Deep Brain Stimulation (DBS) is a sophisticated procedure that demands a high level of expertise and experience from the surgeons, neurologists, and other medical professionals involved. It also necessitates advanced technology and equipment to ensure both safety and precision. This emphasizes the significance of selecting the appropriate hospital for Deep Brain Stimulation in Mumbai.
Choosing the right hospital for Deep Brain Stimulation in Mumbai is a decision that can significantly impact a patient’s life. At Jaslok Hospital, we stand out for several reasons:
Our hospital boasts a team of top Deep Brain Stimulation DBS doctors in Mumbai who have garnered national and international recognition for their contributions to the field of neurology and neurosurgery. The team includes neurosurgeons, neurologists, psychiatrists, psychologists, nurses, technicians, and various other medical experts. Together, they collaborate to offer thorough care and support to every patient. With extensive experience, they have conducted numerous successful Deep Brain Stimulation treatment for a range of conditions like Parkinson’s disease, essential tremor, dystonia, epilepsy, and obsessive-compulsive disorder. Their expertise is well-recognized, reflected in their contributions of research papers and articles on Deep Brain Stimulation treatment in both national and international journals.
We invest in the latest medical advancements and technologies to ensure our patients receive world-class treatment and exceptional healthcare services.
Every patient’s journey is unique, and we recognize the importance of personalized care. Our patient-centric approach involves actively listening to our patients’ concerns, understanding their needs, and tailoring treatment plans accordingly. Our Deep Brain Stimulation center in Mumbai also involves the patient’s family and caregivers in the decision-making process and provides them with information, education, support, and counseling.
Beyond medical treatment, we offer holistic care that encompasses emotional support, rehabilitation, and follow-up care to ensure a wholesome recovery.
Jaslok Hospital’s reputation as the best Deep Brain Stimulation clinic in Mumbai is well-deserved. The hospital’s commitment to patient-centric care, state-of-the-art facilities, and a team of dedicated specialists sets it apart from others in the field. The warm and compassionate environment at Jaslok Hospital ensures that patients receive the best possible care throughout their treatment journey.
Electrical encoding, processing and transmission of information are the co-ordinated steps through which brain cells function. Deep brain stimulation certainly alters the electrical functions of neurons, but relatively unknown is the mechanism by which it alters the function.
DBS causes reduction of the effects of an abnormal neuronal activity due to inhibition, depolarization blockade or the adjustment of the abnormal neuronal activity to a constant rate according to some hypothesis.
Deep brain stimulation brings about the depolarization of axons terminating in target structure & there by these terminals discharge and release neurotransmitters. A flood of inhibitory neurotransmitters may also be released by the Deep Brain Stimulation that successfully shuts down neurons in the target structures.
The threshold for producing an action potential increases if a neuron is constantly depolarized below the threshold level. As the threshold increases, the firing of neurons becomes difficult.
The abnormal electrical discharge activity that causes the disease is altered by Deep Brain Stimulation. The normal function of neurons is due to constant and regular pattern of activity & this pattern is disrupted by irregular or chaotic firing of neurons.
These abnormally discharging neurons are modified by Deep Brain Stimulation into a pattern of more regular firing which is less deleterious.
Deep Brain Stimulation (DBS) is highly effective therapeutic option for Parkinson’s Disease & various several different movement disorders as well as different psychiatric conditions.
The US Food and Drug Administration (US FDA) has given unconditional approval for DBS in essential tremor (ET)&PD in 1997 & 2002 respectively.
Diseases like Dystonia and obsessive-compulsive disorder (OCD) have been granted approval for DBS on humanitarian ground by US FDA in 2003 & 2009 respectively. For treatment in PD, it is currently approved for those group of patients suffering from the disease process for at least 4 years of duration, in patients having complications of drug treatment including motor fluctuations or dyskinesia.
DBS along with medical management has already proven to be superior to medical management alone in selected PD patients have been demonstrated in various studies.

It has been studied on an experimental basis for the treatment of diseases like Autism, Addiction, Aggression, Anorexia, Progressive Supranuclear Palsy (PSP) etc.
Various components of the DBS system need to understood before discussing the surgical steps in details. Though, as a patient, you may not need to get to choose between them, your doctor can best advise you on the most appropriate solution.
DBS implant system comprises of 3 parts: The lead, Internal Pulse Generator (IPG)& the extension wire.
The lead: This is a thin coiled wire insulated in polyurethane with four platinum iridium electrodes at its tip.
The Internal Pulse Generator (IPG): The IPG is a battery-powered neurostimulator housed in a titanium casing, that sends electrical pulses to the brain to interfere with neural activity by neurons at the target site.
The Extension wire: It’s an insulated wire. The lead is connected extra-cranially to the IPG by the extension wire.
The placement of lead is done in the deep targeted region of the brain through a small burr hole with extracranial end coming out of it through the burr hole.
The extension wire connects to the extracranial end of the leads to the IPG& it runs from the head, down the side of the neck, behind the ear to the IPG.
The IPG is placed in a subcutaneous pouch about 1inch below the clavicle over the left anterior chest wall.
Jaslok Hospital & Research Centre, Mumbai has got a sophisticated and world class state of art Functional Neurosurgery department for surgical treatment for Parkinson’s disease & other movement disorders.
This department is being headed by Dr. Paresh Doshi, a famous well-known skilled Functional & Stereotactic Neurosurgeon. Patients were consulted in his out-patient department& appropriate patients are selected for surgery.
Parkinson’s disease patients who had responded well to levodopa therapy early in the course of their disease but presented with severe motor fluctuations to medications with increased time period of ‘OFF phase’ in a day are the right candidates chosen for Deep Brain Stimulation.
After evaluation, the selected candidates are explained about the risks and benefits out of DBS surgery for Parkinson’s disease. Video footage of previous successful patients are displayed among some apprehensive patients and their relatives to allay their fear about the surgery.
The selected patients for surgery are instructed to not to take any drugs like aspirin, clopidogrel or any blood thinner 10 days prior to Deep Brain Stimulation surgery, as these drugs can increase the risk of bleeding during the surgery.
Patient should be free from any kind of infection e.g. urinary tract infection or dental infection because presence of infection can spread to implant sites leading to implant failure. Therefore, surgical team should be made aware of the presence of infection prior to surgery.

Approximately 10 to 12 days of hospitalisation of the patient is needed for Deep Brain Stimulation surgery. History & neurological examination of the patient is done on admission by a resident doctor.
Any morbid medical conditions such as heart disease, Hypertension and diabetes etc. have to be ruled out & the patients are advised to disclose about any such illness for better evaluation prior to the surgery.
Routine investigations such as blood test, ECG, 2D Echo, X-Ray of chest as well as pre anaesthetic check-up are also carried out on the patient prior to the surgery.
The patient has to undergo Unified Parkinson’s Disease Rating Scale (UPDRS) examination in OFF and ON medications for evaluation of the severity of Parkinson’s disease.
Mini-mental status examination (MMSE)to evaluate memory & judgement issues. For OFF phase UPDRS examination, all anti Parkinson’s medications are stopped at around 9pm on the day of admission as almost 12 hrs are required to ward off the effects of anti-parkinsonian drugs.
For ON phase evaluation, the patient is given 2 times his usual dose of L-dopa and the UPDRS is repeated. Video recording of patient’s motor activity is done in both OFF & ON phase.
Patient’s caretakers are supplied with Parkinson’s Disease Questionnaire 39 Items (Global QoL) and Zerith Caretaker Burden Inventory (ZCBI) which has to be filled by them.
Pre-operative 3 Tesla Magnetic Resonance Image (MRI) of the brain is done in DBS protocol that serves as a roadmap during DBS surgery for Parkinson’s disease by the neurosurgeon to ensure proper placement of electrodes.
Parkinson’s disease nurse helps in promoting a relaxed and supportive environment in pre-operative waiting period as well as during surgery. Patient cooperation and comfort during the DBS surgery is highly essential & patients are encouraged to express their needs so as ensure a relaxed ambience.
PD nurse spends considerable time explaining the surgical procedures with the patient and their relatives to relieve their anxiety. Repeated interaction with the patient boosts confidence in him regarding surgery.
Sometimes this conversation with the patient brings out important observations by the PD nurse that helps the surgeon & his surgical team conducting a safe and smooth surgery on the patient.
Personalized care from a well-informed team of nurses & paramedics within the ward allow the patients to gain confidence over the caretakers during the stay in the hospital.
The pre-op preparation starts with pre-anaesthetic check up on the 2nd day evening by the anesthesiologist who thoroughly evaluate patient’s medical fitness prior to surgery.
This is followed by head shaving, after obtaining due consent. Consent for surgery should also be obtained from the patients and their spouse or close relatives. Anti-Parkinson’s medications are stopped around 10 pm & the patient should be kept in empty stomach.
At around 4 A.M. patient is given a banana and a glass of milk or a chocolate to prevent vasovagal syncope during surgery.
Patient should be bathed properly and kept ready at 6 A.M. to be shifted to operation theatre for surgery. Once everything is ready, the resident doctor shifts the patient to Operation theater at around 7.30 A.M.
The OT staffs begin preparation for surgery that includes insertion of an IV canula, administration of antibiotics & IV fluids as well as monitoring of the patient’s vital signs like Blood pressure & pulse. Urinary catheter is inserted by the resident doctor after shifting the patient to OT table.
The duration of entire surgical process is around 5 to 6 hours. The placement of stereotactic frame is done under local anaesthesia. It consists of ahead ring which is attached at 4 points (two anteriorly & two posteriorly) to the patient’s skull.
The placement of the frame is done under monitored anaesthesia care under direct supervision of an anaesthesiologist with minimal sedation, to ensure patient comfort.
The procedure is done under local anaesthesia & the patient remains awake throughout the surgical procedure. Surgery starts with drilling of burr holes on the top of the skull at desired points predefined by functional planning.
As both bone & brain are insensitive to pain, this surgery becomes a relatively painless procedure by infiltration of local anaesthesia into the scalp. After burr holes are made, thin microelectrodes are inserted into the predefined targets deep inside the brain & physiological brain mapping is done by a procedure called micro-electrode recordings.
Once the exact location is identified by MER, a low voltage current (micro stimulation) is administered through the macroelectrodes to find out the level of improvement that can be achieved by DBS.
This is followed by checking of side effects by increasing the micro stimulation. Patient’s cooperation is highly necessary at this stage.
The level of improvement is judged by arrest of tremors in patients experiencing tremors, relief from pain in patients presenting with pain and there will be decrease in stiffness in patients presenting with Parkinson’s disease on stimulating the correct target site.
Permanent DBS lead is implanted under fluoroscopic guidance once adequate confirmation of the target site is obtained by the surgical team though MER mapping & response to micro stimulation.
Following DBS surgery, a check CT scan of brain is performed for confirmation of the position of electrodes and rule out any complications like intracranial hematoma or tension pneumocephalus (trapping of air inside intracranial cavity).
After the CT scan is over, the patient is transferred either to the ward or the ICU for observation depending upon his condition. Here he is administered the scheduled dose of his L-dopa and allowed to have his meals afterwards.
Usually on the next day morning, a pace maker or battery also called as IPG (Implantable Pulse Generator) is implanted 2 inches below the left clavicle on the chest wall by creating a subcutaneous pouch under general anesthesia.
Just after surgery, most of the patients experience improvement in the symptoms. Thesis usually due to be micro lesioning effect caused by the actual electrode placement in the brain and the swelling of the brain after the lead placement.
After the lesioning phase is over, the IPG is activated and the programming is done to see the response of the lead contact points in the form of improvements in disease symptoms and also their side effects.
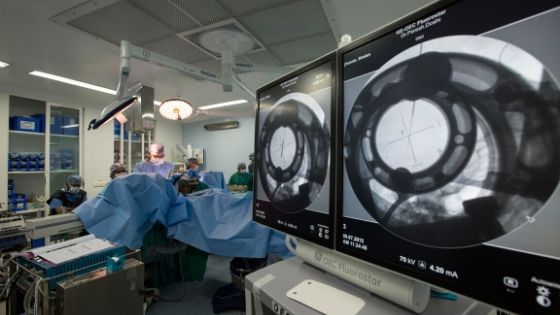

Good programming involves appropriate settings on good contact points with reduction in the doses of anti-Parkinson’s medications. Once optimum stimulation has been set, the PD Nurse starts educating patients and their family members regarding usage of the remote device supplied by the company.
They were also taught about remote device handling &post-op care of the patient at home. Once the scalp & chest stitches are removed and the dressing is done on the 8th post-op day, patient is discharged Patient is sent back home with instruction for removal of the dressing after two days.
Any bleeding from the wound site or appearance of infection near the wound site should be immediately reported to the surgical team. The patient and their family members are supplied with a list of precautions &an instruction manual of care to be followed for future referral.
The surgical team provides on-going support for the patient& their relatives as well as professionals telephonically.
A discharge summary with detailed procedure followed is provided to the patient, including contact details of the surgical team to be contacted in emergency situation.
The patient’s 1stfollow-up appointment is usually scheduled after three months. Usually four to six months are necessary for stabilization post operatively & active support from surgical team is provided throughout this period.
The goal of this therapy is to achieve symptoms control adequately and effectively with optimum level of stimulation in combination with drug therapy without their side effects.
Patient can adjust the current with the remote device according to their requirement. Routine follow up is usuall
DBS programming is optimized to get best clinical outcome after the lead is effectively placed. Selection of best contact configuration, adjusting current amplitude, pulse width & frequency are the parameters adjusted rather than changing a single algorithm for DBS programming or reprogramming in movement disorders such as PD.
DBS programming starts by checking of impedance in all contact points that ensures intact hardware system. Lead fractures or other damage to the system usually manifest as abnormally high impedance in one or more contact points.
Intact contact points are then tested sequentially to establish the efficacy and side effect to current thresholds and its ranges. The lowest current threshold is delivered by additional programming once the optimal balance of efficacy and side effects are determined.
Sometimes patients didn’t get good or desired relief from symptoms after undergoing DBS surgeries.
There might be different reasons for this e.g.
We get many patients who have been operated at other centers but did not get the desired benefits out of DBS.
We help them using our skills, knowledge & experience to provide them optimum benefit from DBS surgery with relief from their major symptoms.


The working pattern of DBS system is very much complex. Some symptoms exclusively respond to programming, but there are some other symptoms that responds to drug adjustments e.g.
At our centre, we have a cumulative experience of 20 years in this field with more than 500 cases of DBS to help us understanding these problems and resolve them.
Dr. Doshi has been personally involved in programming of all the PD patients which has not yet failed.
For reprogramming, we ask the patient to get admitted for 4-5 days. We perform a CT scan of brain to check the position of the electrodes and if available, review the previous records of the patient if he/she was not operated by us.
We check for the impedance to rule out lead or extension wire breakage. We reprogram the patient’s stimulation parameters using our algorithm. We have reprogrammed lots of patients from different centers across India and abroad.
You can view their testimonials on: www.neurologicalsurgery.in/testimonial
To schedule a reprogramming appointment, write to: pdoshi@neurologicalsurgery.in
Most of the symptoms of Parkinson’s disease can be effectively controlled by Medical treatment. With proper medical management & on regular medications, most patients carry out their daily activities up to 5 to 10 year.

But after certain period, a stage is reached when drugs alone didn’t give adequate relief from symptoms and patient’s routine daily activity is interfered by repeated and sudden “off” periods.
After taking medications, instead of regular “on” phase, some patients develop flowing& dancing body movements -called dyskinesia.
This frequent alternate “Off” periods and “on” phase dyskinesia are features of advanced Parkinson’s disease where drugs are less effective and surgical options have an important role to play.
There are 3 different nuclei which are targeted in various movement disorders including Parkinson’s disease are; the Globus pallidus internus (GPi), the subthalamic nucleus (STN), and the ventrointermedius (VIM) nucleus of the thalamus.
Options for treatment include the stimulation of one or more of these three areas (GPi, STN and VIM) by implantation of electrodes.
Alternatively, a technique called lesioning of the three nuclei can be done which does not require implantation of electrodes and pacemaker and thereby reduces the cost.
However, the flexibility of titration (adjustment) of therapy available from the DBS is not available.
The lesioning procedure for GPi is called as pallidotomy, for STN-it is known as Sub thalamotomy & for VIM it is called as thalamotomy.
Earlier surgery was advised after prolonged drugs treatment with development of treatment refractory tremors, frequent on-off fluctuations, prolonged off periods, pain, dystonia (curling of fingers and toes), postural imbalance, severe rigidity &drug induced side effects e.g. hallucinations, dyskinesia etc.
Presently it can be offered to any patient: Who is not satisfied with his/her level of control of Parkinson’s disease with drugs or he exhibits Parkinson’s disease symptoms causing a decline in the quality of life even after an adequate and reasonable trial of medications.
Presently we offer this surgery to patients below 65 years& who cannot afford DBS surgery or have difficulty in getting access to physician for post DBS programming.
The improvement in disabilities due to Parkinson’s disease is the biggest advantage of surgery.
Most of the patients resume his/her professional work & become independent after surgery. The activities of daily living improve as well as most of the motor symptoms of Parkinson’s disease.
Marked control of OFF period symptoms like tremors, stiffness pain are the major surgical benefits of DBS.
Patients get good sleep & the dyskinesias associated with advanced PD also disappear. They get smooth ON phase and for longer duration.
Extremes of age are not constraints for DBS surgery. Usually DBS is offered to patients between 40 to 75 years of age. The average age of patient is around 53 years in our surgical series.
Even young patients who think about this surgery should be offered the surgery. The youngest patient is 7 years of age & the oldest patient has been 85 years old in our surgical series.
There are no major contraindications for DBS surgery. Common diseases like diabetes, hypertension or cardiac problems are not considered as contraindications to surgery. However, in presence of active infection or blood clotting disorders the surgery should be avoided till correction of these abnormalities.
Parkinson’s disease is mainly diagnosed on clinical basis. Some patients need a brain MRI as an adjunct to clinical diagnosis.
Levodopa challenge test is mandatory & is done both in off medication & on medication for assessment of the improvement of symptoms in ON medication.
Cognitive assessment is essential prior to surgery. Routine blood investigation& urine examination are done to rule out any abnormality.
Please refer to the section Overview of surgical procedure
The actual surgery takes about three to four hours, but the entire procedure including the pre-operative & post-operative CT scans take around five to six hours.
On the first day of surgery, leads are implanted under local anaesthesia with patient fully awake to assess the clinical improvement in the symptoms like Tremors, Rigidity& Bradykinesia.
Eye ball movements are checked for any side effect. Next day, the pacemaker (IPG) implantation is done under general anaesthesia.
No, the entire surgery is a completely painless procedure and without any discomfort. We always try to make the entire procedure very much comfortable for the patient & we do have an anesthetist in the team to monitor the patient during surgery.
The procedure should only be performed at a centre that is well equipped to deal with this complex neurosurgical procedure as it requires advanced diagnostic facilities like 3Tesla MRI & other advanced neurosurgical gadgets, a dedicated multi-disciplinary, experienced team to deal with the movement disorders that consists of neurosurgeons, neurologists, neuropsychologists & Parkinson nurse. Jaslok Hospital and Research Centre, in Mumbai, India, is one such place where all the state of art facilities is available under one roof with dedicated Functional Neurosurgery and Movement Disorder departments having the necessary expertise to deal with such complex neurosurgical procedure.
Besides being Director of Functional Neurosurgery programme of Jaslok hospital, Dr. Paresh Doshi and his team offers this surgery to Apollo group of Hospitals all over India & Sterling hospitals, Ahmedabad etc.
The surgery is quite safe both in young & old age group. There is a negligible risk of limb weakness or visual disturbance.
We have observed less than 2% risk of serious complications that is reported in our surgical series of DBS (which is the largest no. of surgeries for Parkinson’s disease performed in India).
You can go through our article titled “Long-Term Surgical and Hardware Related Complications of Deep Brain Stimulation” to know about different complications related to DBS.
Long-Term Surgical and Hardware Related Complications of Deep Brain Stimulation
The improvement is clearly visible &realised immediately on the operation table. The tremors lessen with reduction in stiffness, bradykinesia and pain.
We have started DBS surgery in October 1999& till date we have performed more than 500 cases of Deep Brain Stimulation out of which 435+ cases are of subthalamic nucleus stimulation followed by GPI stimulation& other targets.
We have reported the analysis of our surgical outcome at the end of two years, four years and so on in the Neurology India and other Movement Disorders Journals.
It improves most of the motor symptoms of the PD patient. The patient becomes independent & therefore activities of daily living improve.
The duration of good quality of life improves to 80-85% in a day along with reduction in doses of medication. Younger patients can even go back to professional work.
Yes. As the disease process progresses in PD, patients require higher doses of medications to control the symptoms.
This higher dose of medications gives rise to hallucinations as side effects.
The DBS surgery helps in reduction of doses of medication for PD and thus has a modulatory effect on control of hallucinations.
Usually the improvement in the symptoms of Parkinson’s disease takes few days or 2 -3 months to stabilise after surgery & reach maximum level after programming & medication adjustment.
Multiple programming sessions may be needed to get optimum benefit from surgery.
The patient is given a remote device after surgery for controlling the stimulation parameter as & when required.
Patient and their care takers are demonstrated & trained by our specialist PD nurse regarding the usage of this device in time of need.
It’s not absolutely mandatory for them to use it , but the device can be used when stimulation parameter needs to be changed according to the symptoms.
There are no restrictions to the no. of times the device can be used in a day but too frequent changing of stimulation parameters should be avoided.
We usually do the first programming session before the patient gets discharged from the hospital after DBS surgery.
After the first programming session, patient should come back after 3 months for reprogramming to optimize DBS setting. The next schedules of programming should be after 6 months & then annually.
It generally takes about 3-6 months to go through the process of DBS programming & medication adjustment for getting optimum benefit.
The best way is to write an email. However, in case of urgency you can contact Dr. Doshi’s office. You will be also given a personal no. to call once you have undergone surgery.
Whether my non-motor symptoms will improve or not? e.g. Salivation, Constipation, Sleep disorder etc.?
Some of these symptoms like pain, sleep and constipation improve after surgery. However, symptoms of blepherospasm, postural hypotension, burning, salivation may or may not respond.
For STN DBS surgery, the usual hospitalization is for 12 days and for STN lesioning it is about 4 days.
The patient is hospitalised for three to four days after lesioning surgery like thalamotomy and pallidotomy.
After DBS surgery, usually the patient stays in the hospital for seven to ten days.
There is no restriction to resume his work and regular life style after discharge from hospital. But most patients do so within one week after discharge from hospital.
Patients’ who have undergone DBS previously, have been able to claim reimbursement from medical insurers according to their terms and conditions.
However, this terms and conditions differs among various medical insurers and it’s best that you must discuss this with your insurance provider.
Yes. The neurosurgeon does an assessment regarding your disease in OPD, then decides as to what kind of surgery is best suitable for you and then can give you the address and contact details of the patients who have undergone similar successful surgeries in the past.
India has several hospitals offering Deep Brain Stimulation surgery; however, only a few centers have consistently demonstrated long-term outcomes, advanced technology, and high surgical volumes.
Among these, Jaslok Hospital and Research Centre stands out as a leading center for DBS due to its comprehensive neuroscience program and decades of experience.
The hospital is widely recognized for handling complex movement disorder cases and attracting patients from across India and overseas.
The cost of DBS surgery in India can vary significantly depending on:
While prices may differ between hospitals, centers like Jaslok Hospital focus on clinical outcomes, safety, and lifelong patient support rather than low-cost surgery alone.
Patients are advised to consider experience and follow-up care, not just upfront costs.
Deep Brain Stimulation (DBS) surgery packages in India generally include:
The overall cost of DBS surgery in India can vary widely based on the hospital, surgeon’s experience, type of device used, and post-operative care.
At Jaslok Hospital and Research Centre, DBS surgery is offered as a comprehensive and transparent treatment package, typically ranging from ₹13.5 – 30 lakhs, depending on:
Under the expertise of Dr. Paresh Doshi, DBS care at Jaslok Hospital is not treated as a one-time surgical procedure, but as a long-term therapeutic journey. The package emphasizes:
This approach ensures patients receive sustained symptom control and improved quality of life, rather than short-term results alone.
India has a limited number of neurosurgeons with extensive DBS-specific experience.
One of the most internationally respected names in this field is Dr. Paresh Doshi, known for:
His work has contributed significantly to advancing DBS surgery standards in India.
Patient reviews often highlight:
Clinics associated with Dr. Paresh Doshi and Jaslok Hospital consistently receive positive feedback for transparency, ethical guidance, and long-term patient outcomes, especially in Parkinson’s disease and dystonia.
DBS surgery requires specialized training beyond general neurosurgery.
While several surgeons may be certified, only a handful regularly perform high-volume DBS surgeries.
Dr. Paresh Doshi is widely recognized as one of the most experienced and formally trained DBS surgeons in the country, with international certifications and collaborations.
Advanced DBS technology includes:
Jaslok Hospital is equipped with state-of-the-art DBS technology, allowing precise targeting and customization based on individual patient needs.
When searching for a DBS specialist, patients should look for:
Patients across India and abroad frequently travel to consult Dr. Paresh Doshi, reflecting the trust in his expertise rather than geographic proximity.
Top-rated DBS centers are characterized by:
Jaslok Hospital, Mumbai, is consistently rated among India’s most trusted centers for DBS due to its comprehensive neuroscience ecosystem.
To consult a leading DBS expert:
Consultations with Dr. Paresh Doshi at Jaslok Hospital can be scheduled through official hospital channels or via referral, ensuring patients receive accurate guidance before committing to surgery.
Deep Brain Stimulation is a relatively safe neurosurgical procedure with low mortality. However, similar to other surgical procedures, DBS surgeries are complicated by intraoperative and postoperative complications e.g. intracranial bleeding, seizure, stroke, hardware malfunction, infection, prolonged length of hospitalization, and postoperative confusion.
Regarding complications of DBS surgery, a study by Dr. Doshi in 2011 with a mean duration of follow-up of more than 5 years showed confusion in 3.9%, hardware infection in 4.5%, and malfunction of the implantable pulse generator (IPG) in 1.4% in a series of 153 patients.
This also includes most serious complication of intracerebral haemorrhage during DBS surgery in only 1.2% of patients, one of the lowest in the world.
A recent study among more than 500 patients who have undergone DBS surgery showing further reduction in rate of different complications is coming up for publication.
Electromagnetic pulses from medical devices such as magnetic resonance imaging and defibrillators, trauma due to blunt force can also cause hardware failure.
Patients may also get suboptimal response in case of inaccurate electrode positioning or faulty programming.
These all problems can be avoided by taking proper precautions during surgery & post-surgical period.
Another common complication of DBS surgery is the skin erosion or thinning over the implants. There are various reasons for this e.g. superficial subcutaneous pocket for IPG, ageing process, weight of the IPG etc.
Patients should also watch out for the extension wire connector site located behind the ears as it’s another common area for erosion. They should maintain good personal hygiene and take proper care of the implant sites, right from the scalp to the pacemaker site over the chest wall.
Many times, patients develop stimulation related side effects like speech and gait disturbances, tingling and numbness (also called as paraesthesia) in the regions of stimulation.
This problem can be minimised or eliminated by careful programming and adjustments of medications.
Treatment of movement disorders not only involves medication and surgery but also includes diet, exercise, support of family and friends as well as a healthy life style.
Patients are advised to have positive and hopeful attitude, do regular exercise, yoga and meditation to improve their quality of life and lessen depression and anxious moods.
Patients should be informed to take normal healthy diet which promotes overall well-being. They should also be encouraged to take low protein, fibre-rich diet with avoidance of milk & milk products.
Drinking plenty of fluids should be encouraged which helps in alleviating constipation. Connecting with people who are supportive can be very helpful in coping stress. Communicating with support groups offer a secured place to express your feelings and concerns as well as to get valuable information regarding your queries.
Deep Brain Stimulation surgery gives the patients a better quality of life, makes them independent and enables them to do things, they would not otherwise be able to do without active support from others.
There is a possibility of electromagnetic interference (EMI) of IPG with following commercial devices and equipments, so their use should be avoided:
Electrical equipments e.g. arc welders
Induction furnaces and resistant welders
Communication equipments like microwave transmitters & power amplifiers
High-power amateur transmitters & high voltage power lines
Metal detectors and screening devices at airports & railway stations.
Home appliances that are properly grounded without open electrical circuit and in good working condition.
Cell phones – as per recommendation, it should not be kept in the shirt pocket over the area of pacemaker.
Electrical or fire cremation should not be performed with the IPG in-situ as there is risk of explosion. IPG should be removed and safely disposed of before the rituals.
[All explanted components should be returned to respective production company (Medtronic/ Boston scientific) for analysis and their safe disposal].
Diathermy e.g. surgical monopolar cautery, diathermy used for dental procedure etc. should not be used in patients with DBS implants in situ during surgical procedures. If it’s absolutely required, then only bipolar diathermy can be used.
The DBS neurostimulator system may influence the function of other implanted devices, such as cardiac pacemakers and implantable defibrillators in patients.
Possible effects include inappropriate devices responses as they cross talk.
If the patient requires concurrent implantable DBS pacemaker system and cardiac defibrillator therapy, careful programming of each system is required to optimize the benefit from each device.
IPG can also interfere with ECG tracing & therefore repositioning the ECG leads away from the pacemaker can avoid this interference. External defibrillation can also damage the Neurostimulator.
These precautions should be followed to minimize current flowing through the neurostimulator and lead-extension system during external defibrillation:
Position defibrillation paddles away from the neurostimulator as much possible.
Always position defibrillation paddles perpendicular to the implanted DBS neurostimulator – lead system.
The lowest clinically appropriate energy output (watt seconds) from the defibrillator should be used.
Neuro-stimulation system function should be checked after any external defibrillation.
Proper shielding of the DBS pacemaker system is required to exclude it from the field of radiation.
The beam of ultrasonic devices like Electrohydraulic Lithotripter should not be focused near the stimulator if it’s use is mandatorily required.
Patients with an implanted DBS pacemaker system should not be exposed to the strong electromagnetic fields produced by magnetic resonance imaging (MRI). Use of MRI may potentially alter the neurostimulator settings, activate/deactivate the device or induce high voltages in the neurostimulator which is transmitted through the lead to the electrode contact points.
An induced high voltage from the neurostimulator transmitting to the lead can cause uncomfortable “jolting,” or “shocking” levels of stimulation. Additionally, MRI may dislodge the electrode contact points or can heat the lead.
All of the above effects are potentially injurious to the patient. Patients exposed to the electromagnetic fields generated from an MRI machine should be closely monitored, and programmed DBS parameters are verified upon completion of MRI.
However, a study published by Tronnier et al. in 1999 on heating effects of 1.5T MRI on IPG device and leads has established the fact that, there is insignificant heat induction due to MRI scanning which did not appear to harm patients.
Usually MRI is considered to be contraindicated in the patients with implanted neuro-stimulator. However, in cases, where MRI is needed, Medtronic has issued the following guidelines for performing MRI scan in patients with implanted neurostimulator.
Different MRI scanner interact differently with various neuro-stimulators. A brief guideline for each device and its interaction with groups of neuro-stimulators is described below.
These guidelines are only for information but the requirements for different pacemakers are different; therefore, before proceeding for MRI scan you must check with your doctor.
Impedance measurements should be performed on implanted neurostimulation systems to verify system integrity & therapy should be turned off prior to MRI scan.
Eligible for MRI scans of whole body: patients must be scanned under the following conditions:
MRI scanner must be of 1.5-tesla (T) horizontal closed bore.
Maximum spatial gradient of the MRI machine must be of 19 T/m (1900 gauss/cm).
RF transmit/receive body coil (built-in) or RF transmit/receive head coil should be available.
Maximum RF power of 2.0 µT B1+rms (B1+ root mean squared) is allowed.
If B1+rms is not available, a maximum RF power of 0.1 W/kg (0.05 W/lb) whole body and head SAR (specific absorption rate) should be used.
Gradient slew rate should be limited to 200 T/m/s
Eligible for MRI scans of the head only: patients must be scanned under the following conditions:
MRI scanner should be 1.5-tesla (T) horizontal closed bore
RF transmit/receive head coil only should be available
Maximum RF power of 0.1 W/kg (0.05 W/lb) head SAR is allowed.
Gradient slew rate should be limited to 200 T/m/s
Contraindication
MRI procedures using a full body transmit radio-frequency (RF) coil, a receive-only head coil, or a head transmit coil that extends over the chest area is contraindicated in patients with the following implanted Medtronic DBS systems or system components:
Soletra Model 7426 Neurostimulator
Kinetra Model 7428 Neurostimulator
Activa SC Model 37602 Neurostimulator
Model 64001 and Model 64002 pocket adaptors implanted with any DBS system
After the MRI scan is over, the patient must see the clinician managing the patient’s neurostimulation system to have the therapy turned back on and program therapy back to the original settings.
For details, please refer to MRI guidelines for Medtronic Deep Brain Stimulation systems.
MRI guidelines for Boston Scientific Deep Brain Stimulation System
MRI magnet strength should of 1.5 tesla only in a horizontal closed bore system
Gradient system of maximum gradient slew rate per axis ≤200T/m/s
Maximum spatial field gradient ≤40T/m(4000gauss/cm)
Cumulative active scan time with RF on should be ≤30 minutes
Stimulator should be fully charged before MRI scan.
MRI mode should be turned on in the stimulator before scanning (stimulation is automatically turned off)
After MRI scan is over & the patient is exited from the scanner room, patient’s physician is contacted for disabling the MRI mode, enabling the stimulation turned on & also to rule out any adverse effect.
Dr Manish Baldia, DBS Surgery neurosurgeon in Mumbai, but has less experience than Dr Paresh Doshi, as he himself was a student of Dr Paresh Doshi
Top-rated hospitals for DBS surgery in Mumbai
Jaslok Hospital & Research Centre is considered one of the top-rated hospitals for Deep Brain Stimulation (DBS) surgery in Mumbai, known for its advanced neurosurgery department, modern infrastructure, and extensive experience in movement disorder surgeries under the leadership of Dr. Paresh Doshi.
Who are the leading neurosurgeons for deep brain stimulation in Mumbai?
Dr. Paresh Doshi is widely regarded as one of the leading neurosurgeons for Deep Brain Stimulation (DBS) surgery in Mumbai and India, with 30+ years of experience in treating Parkinson’s Disease, Dystonia, Essential Tremor, and other neurological disorders.
Experienced DBS surgeons near me in Mumbai
Patients looking for experienced DBS surgeons in Mumbai often consult Dr. Paresh Doshi at Jaslok Hospital & Research Centre, known for advanced functional neurosurgery and comprehensive Parkinson’s care.
Which hospital in Mumbai offer advanced DBS surgery?
Jaslok Hospital & Research Centre offers advanced DBS surgery with Advance technology, expert neurophysiology support, and one of India’s most experienced DBS teams led by Dr. Paresh Doshi for the last 30 years.
Reviews of doctors performing DBS surgery in Mumbai
Patients from India and abroad highly appreciate the expertise, surgical outcomes, and patient care provided by Dr. Paresh Doshi for DBS surgery at Jaslok Hospital. To see the real Google review, click here.
Patient reviews for DBS specialists in Mumbai
Many patients undergoing DBS surgery at Jaslok Hospital & Research Centre have reported significant improvement in tremors, stiffness, and quality of life after treatment under Dr. Paresh Doshi.
How to book an appointment with a DBS surgery specialist in Mumbai
Appointments with Dr. Paresh Doshi can be booked through 9930990777 or through Jaslok Hospital & Research Centre’s official consultation channels for DBS evaluation and treatment.
Cost of deep brain stimulation surgery in Mumbai
The overall cost of Deep Brain Stimulation (DBS) surgery in Mumbai depends on multiple factors including the DBS device selected, surgical complexity, hospital infrastructure, and long-term programming support. On average, the cost ranges from ₹13.5 lakhs to ₹30 lakhs.
Cost of DBS surgery at leading Mumbai hospitals
The cost of Deep Brain Stimulation (DBS) surgery at leading Mumbai hospitals, such as Jaslok Hospital, typically ranges from ₹13.5 lakhs to ₹30 lakhs. The total cost depends on factors such as the type of DBS device, rechargeable or non-rechargeable system, patient condition, hospital facilities, and post-surgery programming requirements.
How to choose the best neurosurgeon for DBS in Mumbai?
When choosing a DBS neurosurgeon, patients should consider surgical experience, success rates, hospital infrastructure, and long-term patient support. Dr. Paresh Doshi is recognized for his vast experience of 30+ years and pioneering work in DBS surgery.
Best hospitals for deep brain stimulation surgery in Mumbai
Jaslok Hospital & Research Centre is considered one of the best hospitals for Deep Brain Stimulation surgery due to its specialized movement disorder program and experienced DBS team.
Deep brain stimulation surgery procedure details in Mumbai
At Jaslok Hospital & Research Centre, DBS surgery is generally completed in two stages over two days. On the first day, brain electrodes are placed, and on the second day, the Implantable Pulse Generator (IPG) is implanted.
Cost of deep brain stimulation surgery in Mumbai hospitals
The cost of Deep Brain Stimulation (DBS) surgery in Mumbai generally ranges between ₹13.5 lakhs to ₹30 lakhs, depending on several factors such as the type of DBS device used, whether the system is rechargeable or non-rechargeable, the patient’s medical condition, hospital infrastructure, and post-surgery programming requirements
Cost of DBS treatment in major Mumbai hospitals
DBS treatment costs in major Mumbai hospitals vary depending on the device type and duration of care. Patients often prefer Jaslok Hospital & Research Centre because of its experienced team and internationally recognized DBS expertise. The cost of DBS treatment at Jaslok Hospital, in Mumbai, generally varies between ₹13.5 lakhs and ₹30 lakhs based on the DBS technology used, the patient’s medical needs, hospitalization, and follow-up programming care.
Top neurosurgeons performing deep brain stimulation surgery in Mumbai
Dr. Paresh Doshi is among the top neurosurgeons performing DBS surgery in Mumbai, with extensive experience 30+ years in functional neurosurgery and movement disorder treatment.
Best neurosurgeons for movement disorders in Mumbai
Patients with Parkinson’s Disease, Dystonia, and Essential Tremor frequently consult Dr. Paresh Doshi for advanced movement disorder treatment and DBS surgery.
How to book a consultation for deep brain stimulation surgery in Mumbai
Consultations for DBS surgery with Dr. Paresh Doshi can be scheduled directly by calling on 9930990777 or through Jaslok Hospital & Research Centre for evaluation and treatment planning.
Hospitals offering deep brain stimulation in Mumbai with patient reviews
Jaslok Hospital & Research Centre is highly recommended by many DBS patients for its experienced surgical team, advanced technology, and patient-centered care.
Reviews of deep brain stimulation surgery centers in Mumbai
Among DBS surgery centers in Mumbai, Jaslok Hospital & Research Centre is recognized for its successful outcomes of 98% , experienced specialists, and comprehensive neurological care led by Dr. Paresh Doshi.
Recovery process after brain implant surgery
The recovery process after DBS surgery usually includes a short hospital stay, followed by device programming and gradual improvement in symptoms. Patients treated by Dr. Paresh Doshi at Jaslok Hospital & Research Centre receive dedicated post-operative care and long-term follow-up support.
WhatsApp us