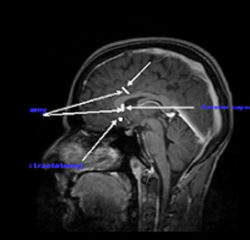
In 1947 stereotactic neurosurgery was developed, reducing considerably many post-operative adverse effects and complications. Since then, different centers have started to employ several stereotactic techniques, such as anterior cingulotomy (US), capsulotomy (Sweden), subcaudate tractotomy and limbic leucotomy (England and Australia).
Afterwards, Leksell simulated capsulotomy lesions focusing gamma rays beams emitted by Cobalt-60 radioactive isotope on the internal capsule. Large number of surgeries was performed during this time i.e. during 1940-1960s as there was no medical treatment for these disorders. However, with the availability of newer drugs the number of surgeries decreased. Recently, due to the better understanding of the disease and improved safety of surgical procedures, the interest in surgical treatment has reappeared.
Overview of surgical targets and technique
Appropriate selection of patients for surgery remains a major issue and the responsibility of the psychiatrist, guided by the informed and expert opinions of the other members of the psychosurgical team. Ethical objections of psychiatric neurosurgery are addressed in all centers by ensuring an informed consent from the patient and family.
Patient Selection
The selection criteria that we adopt are derived from distillation of various randomized study around the world. These have been further reaffirmed by the “National Advisory Committee for Psychosurgery in India” committee that met on 8th March 2009. The following guidelines have been adopted for selection of patients:
- Detailed patient screening, record review, interviews with the treating clinicians and baseline assessments, including the Structured Clinical Interview for Diagnostic and Statically Manual of Mental disorders 4thedition, should be used to assure that OCD is the primary diagnosis
- OCD for at least 5 years duration
- YBOCS symptom intensity in the ‘severe’ range was required (score 28 or more)
- OCD causing marked impairment with a GAF score of 45 or less
Treatment resistance
- This is defined as adequate trial (>3 months) with maximally tolerated doses of at least three serotonin reuptake inhibitors (SRIs), one of which has to be clomipramine.
- Trials combining an SRI with additional medications (including a neuroleptic and a benzodiazepine) should also be tried.
- Minimum of 20 CBT or failure to undertake CBT